Telling obese women to lose weight before trying to have children through fertility treatment may be unnecessary, research suggests.
NHS bosses often tell overweight women who are struggling to conceive to lose weight because carrying excess body fat is linked to reduced fertility.
But now experts say losing weight might not make a difference, according to the first randomized controlled trial of its kind.
Scientists at Penn State University compared fertility treatment success rates among 300 obese women who were struggling to get pregnant.
Half of them followed a 16-week weight loss and exercise program and were only allowed to eat 1,200 calories a day. They were compared to a control group who were told to continue eating as they normally would.
There was no significant difference in pregnancy success rates between the two groups after three treatment cycles – although the calorie-restricted group lost 1 pound (7 kg) on average.
Dr Richard Legro, who led the study, said the results showed “there just isn’t enough evidence” to recommend rapid fat loss before conceiving.
But he acknowledged there were likely “long-term benefits” to fertility fitness.

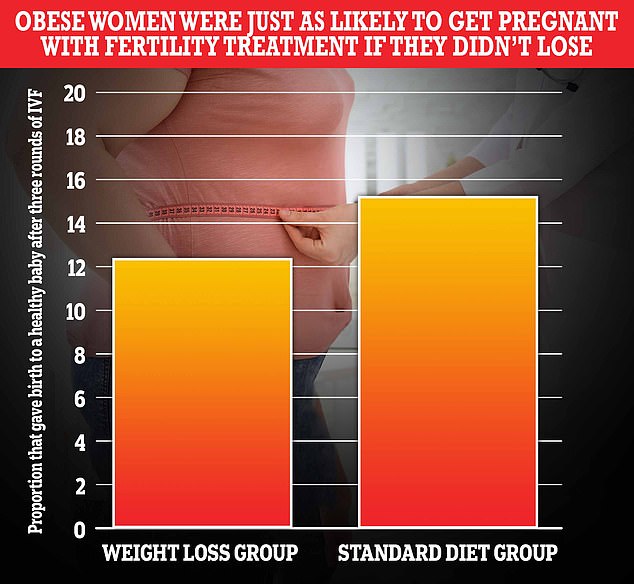
The graph above shows the proportion of obese women who followed a strict 16-week diet (left) and gave birth healthy, compared to the group who did not follow a weight loss plan (right) . Scientists said there was no significant difference between the two groups
On average, even the women who lost weight still weighed 15 pounds (100 kg) after the diet and had a BMI of 36.6, which meant they were still medically obese.
The study did not examine obese women who reach a healthy weight before trying to conceive.
Around one in eight couples in the UK and US struggle to conceive. More than a quarter of Britons are obese and four in 10 Americans are overweight.
The latest study – conducted over a four-year period to September 2019 – included 379 obese women who had been trying for a baby for at least a year without success.
They were between 18 and 40 years old and weighed an average of 16 pounds (107 kg) at the start of the study.
Their BMI was around 39.3, which puts them just below the morbidly obese threshold of 40.
The women and their partners underwent a medical examination before the study and were found to be in good sexual health.
The women were split into two equal groups, with one following a 1,200-calorie diet that included two servings of fruit, three vegetables and two servings of low-fat dairy – such as cottage cheese – per day.
Women in both groups were asked to gradually increase their daily steps from 6,000 to 10,000 per day by the end of the trial.
Those in the calorie-restricted group lost an average of 7% of their body weight, or the equivalent of 1 stone 1 lb (7 kg).
But those in the control group remained at about the same weight.
After 16 weeks, both groups of women were offered three cycles of ovarian stimulation and intrauterine insemination – when sperm is injected directly into the uterus to facilitate fertilization.
This is different from IVF treatment, where an egg is fertilized in a test tube before being implanted in the uterus.
Among the women who lost weight, there were 23 healthy babies (12% success rate), and for those who did not lose weight, there were 29 babies (15%).
The researchers said it was not statistically different.
Dr Legro, who is also chairman of the college’s department of obstetrics and gynecology, told MailOnline: ‘I know the party line on weight loss and pregnancy outcomes, I just stopped believe it when I saw the science.”
“It is difficult for me to tell an obese patient that losing weight just before pregnancy will improve her pregnancy outcome and that of her baby.”
He added: “There are probably long-term metabolic benefits…but the short-term pregnancy benefits aren’t there.”
‘So no, I don’t think the weight loss is necessary. I would stress the importance of preventing obesity in children and adolescents as the best medicine.
Dr Raj Mathur, head of the British Fertility Society who was not involved in the research, said the article raised questions about whether denying obese people fertility treatment was justified.
He told MailOnline: ‘This study encourages us to look at outcomes in patients planning IVF treatment, and also to consider whether a rigid BMI of 30 is justified for the purposes of NHS eligibility.’
“In my opinion, a more flexible approach that allows for discussion between clinician and patient makes more sense.”
It was published in PLOS MEDICINE.
.